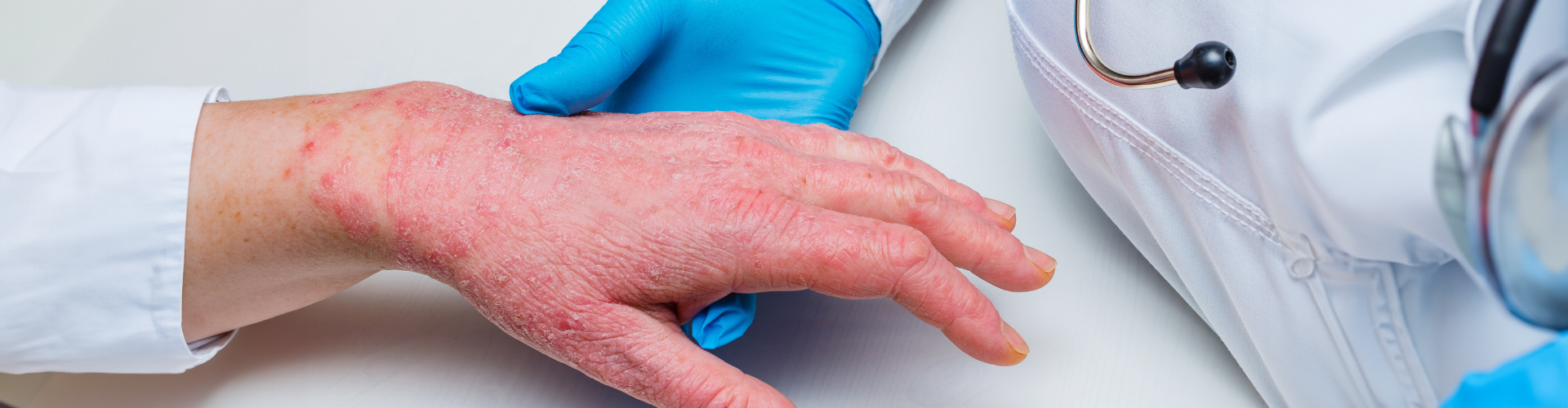
TYPE IV ALLERGIES:
REDUCING THE RISK OF SENSITIZATION WITH DPG- FREE GLOVES
Skin diseases are one of the most common occupational illnesses in Europe.¹
The primary among these is contact dermatitis², which can be divided into irritant toxic and allergic contact dermatitis ( Type I V allergy).
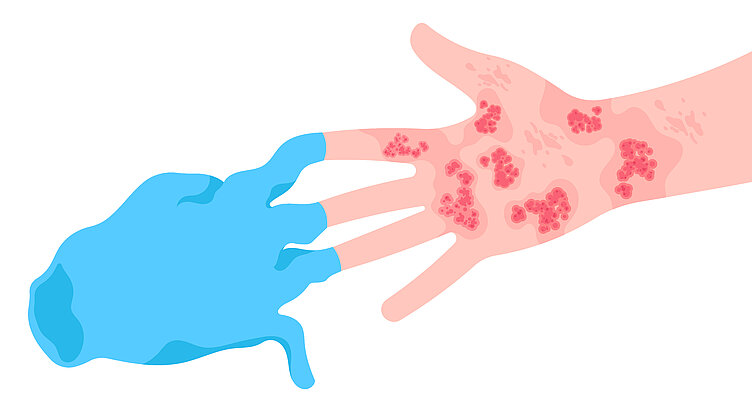
Allergic contact dermatitis
Allergic contact dermatitis (ACD) is triggered by a cellular immune reaction. Approximately 20% of the population have a predisposition to this condition.³ ⁴ ⁵
ACD often results in skin redness (erythema), itching, or burning eczema. In sensitized patients, the onset of symptoms typically takes 24 to 48 hours.
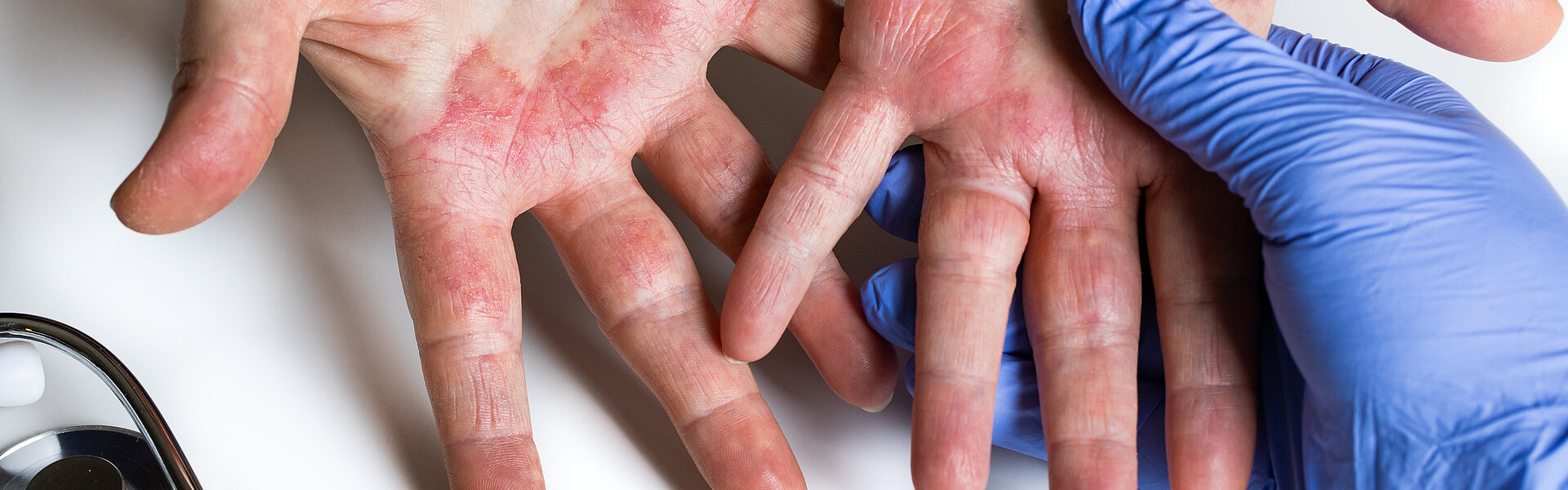
Contact dermatitis accounts for 95% of work-related skin diseases.² It is prevalent in the healthcare sector³, with nurses and nursing assistants accounting for the largest share at 40%, followed by medical assistants (22%) and physicians (18%).⁶
Our synthetic and DPG-free portfolio
Synthetic polyisoprene (IR) is chemically identical to natural rubber and therefore has the same physical properties as natural rubber. It is therefore ideal for the production of skin-friendly gloves, provided that
appropriate accelerators are used.
HARPS Global exclusively offers DPG-free products in its portfolio and does not use Thiurams in glove production.
OUR DPG- AND LATEX-FREE PORTFOLIO
For our conventionally crosslinked products (syntegra IR and syntegra green), we use an accelerator system consisting of a long-chain accelerator (from the dithiocarbamate group) in combination with a thermo-reactive molecule that decomposes residue-free during manufacturing.
For highly sensitized users, we offer a product (syntegra UV) that completely avoids the use of vulcanization accelerators. Instead, crosslinking is achieved through UV light. This product is therefore ideal for people with Type IV allergies.
You want to know more?
Read our brochure and learn more about DPG.
References
¹ Bauer, A., Pesonen, M., Brans, R., Caroppo, F., Dickel, H., Dugonik, A., Filon, F. L., Geier, J., Arnau, A. G., Napolitano, M., Patruno, C., Rustemeyer, T., Simon, D., Schuttelaar, M. L. A., Śpiewak, R., Stingeni, L., Vok, M., Weißhaar, E., Wilkinson, S. M., . . . Uter, W. (2023). Occupational contact allergy: The European perspective–Analysis of patch test data from ESSCA between 2011 and 2020. Contact Dermatitis, 88(4), 263–274. https://doi.org/10.1111/ cod.14280https://doi.org/10.1111/cod.14280
² Bains, S. N., Nash, P. & Fonacier, L. (2018). Irritant contact dermatitis. Clinical Reviews in Allergy & Immunology, 56(1), 99–109. doi.org/10.1007/s12016-018-8713-0
³ Pesonen, M., Jolanki, R., Filon, F. L., Wilkinson, S. M., Kręcisz, B., Kieć-Swierczyńska, M., Bauer, A., Mahler, V., John, S. M., Schnuch, A. & Uter, W. (2015). Patch test results of the European baseline series among patients with occupational contact dermatitis across Europe – analyses of the European Surveillance System on Contact Allergy network, 2002–2010. Contact Dermatitis, 72(3), 154–163. doi.org/10.1111/cod.12333
⁴ Alinaghi, F., Bennike, N. H., Egeberg, A., Thyssen, J. P. & Johansen, J. D. (2018). Prevalence of contact allergy in the general population: A systematic review and meta‐analysis. Contact Dermatitis, 80(2), 77–85. doi/10.1111/cod.13119
⁵ Krob, H., Fleischer, A. B., D’Agostino, R. B., Haverstock, C. L. & Feldman, S. R. (2004). Prevalence and relevance of contact dermatitis allergens: A meta-analysis of 15 years of published T.R.U.E. test data. Journal Of The American Academy Of Dermatology, 51(3), 349–353. doi.org/10.1016/j.jaad.2003.11.069
⁶ Huang, C. H., Greig, D. & Cheng, H. (2021). Allergic contact dermatitis in healthcare workers. Occupational Medicine, 71(6–7), 294–297. https://doi.org/10.1093/occmed/kqab118 Allergic contact dermatitis in healthcare workers. Occupational Medicine, 71(6–7), 294–297. doi.org/10.1093/occmed/kqab118
⁷ Dejonckheere, G., Herman, A. & Baeck, M. (2019). Allergic contact dermatitis caused by synthetic rubber gloves in healthcare workers: Sensitization to 1,3‐diphenylguanidine is common. Contact Dermatitis, 81(3), 167–173. doi.org/10.1111/cod.13269
⁸ Baeck, M., Cawet, B., Tennstedt, D. & Goossens, A. (2012). Allergic contact dermatitis caused by latex (natural rubber)‐free gloves in healthcare workers. Contact Dermatitis, 68(1), 54–55. doi.org/10.1111/j.1600-0536.2012.02054.x
⁹ Cao, L., Taylor, J. S., Sood, A., Murray, D. A. & Siegel, P. D. (2010). Allergic Contact Dermatitis to Synthetic Rubber Gloves. Archives Of Dermatology, 146(9). doi.org/10.1001/archdermatol.2010.219
¹⁰ Geier, J., Lessmann, H., Mahler, V., Pohrt, U., Uter, W. & Schnuch, A. (2012). Occupational contact allergy caused by rubber gloves – nothing has changed. Contact Dermatitis, 67(3), 149–156. doi.org/10.1111/j.1600-0536.2012.02139.x
¹¹ Geier, J., Lessmann, H., Uter, W. & Schnuch, A. (2003). Occupational rubber glove allergy: results of the Information Network of Departments of Dermatology (IVDK), 1995-2001. Contact Dermatitis, 48(1), 39–44. doi.org/10.1034/j.1600-0536.2003.480107.x
¹² Pontén, A., Hamnerius, N., Bruze, M., Hansson, C., Persson, C., Svedman, C., Andersson, K. T. & Bergendorff, O. (2012). Occupational allergic contact dermatitis caused by sterile non‐latex protective gloves: clinical investigation and chemical analyses. Contact Dermatitis, 68(2), 103–110. doi.org/10.1111/cod.12010
¹³ Crépy, M. (2016). Rubber: new allergens and preventive measures. European Journal Of Dermatology, 26(6), 523–530. doi.org/10.1684/ejd.2016.2839
¹⁴ Services, D. O. H. A. H., Prevention, C. F. D. C. A. & Health, N. I. S. A. (2013). Effects of Skin Contact with Chemicals: What a Worker Should Know. CreateSpace.


